What Is Credentialing Software?
Healthcare credentialing software is essential for healthcare facilities, insurance companies, and other organizations that manage the process of ensuring healthcare providers as they keep track of and maintain the proper licenses and certificates to practice medicine. In addition, they aid with the overall ability to properly care for patients. The software even monitors professional requirements and stores a wide range of data about providers.
The software is often referred to as healthcare provider credentialing software or simply provider credentialing software. It is frequently considered part of a credentials management system.
Why Credentialing Is Becoming Increasingly Important
Credentialing is essential for healthcare organizations to ensure providers are properly licensed and can provide reliable healthcare.
Experts say credentialing will become even more important amid the healthcare system’s continuing reform. Ongoing changes in the system will require the following:
- A Shift Toward Longer-Term Goals: Healthcare organizations will need to move toward both longer-term goals for each patient’s overall health and broader goals for population health (as opposed to getting paid to perform a single healthcare service for a single patient). Healthcare organizations will need the appropriate number of providers in various geographic areas to serve the population — which means they need a credentialing process that is smooth and efficient to get doctors working quickly.
- More Intensive Healthcare Services in Hospitals: Organizations will have to move less-urgent health care services out of hospitals when they can be done as well or better in other settings. This will require them to quickly credential healthcare providers in a wide range of healthcare locations.
Who Manages the Credentialing Process?
Most hospitals and healthcare facilities have credentialing departments that ensure all healthcare providers working (or planning to work) at the facility have the requisite credentials. Smaller medical clinics may have just one person in charge of the process. Physicians in solo practice may do the credentialing work themselves.
Healthcare facilities generally follow one of three models (or a combination thereof) to perform credentialing:
- Have staff members perform the work themselves, through direct communication with licensing and other agencies.
- Hire an outside organization (called a credentials verification organization, or CVO) to do some or all of the work.
- Have staff members use credentialing software to help perform the work.
It’s important for healthcare facility leaders to know that hiring a CVO does not absolve them of the ultimate responsibility for proper credentialing. Facilities must continually check that CVOs are doing a good job, often through the use of regular and standard audit tools.
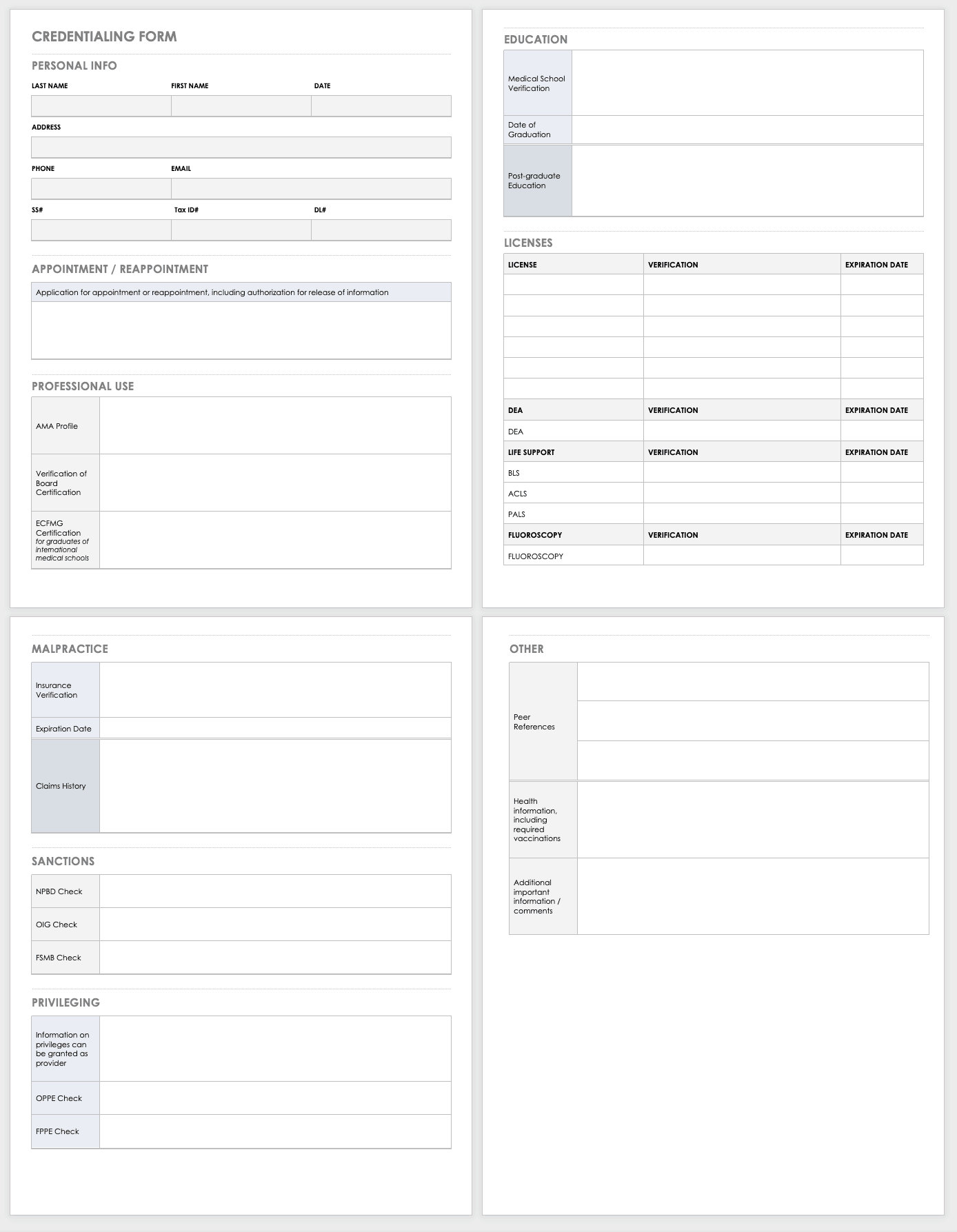
Credentialing Software Template
To ensure you have all the requisite documentation when credentialing a healthcare provider, consider using a checklist. You can download the following template for free and edit it to suit your particular needs.
Download Credentialing Form Template
Excel | Word | PDF | Google Docs
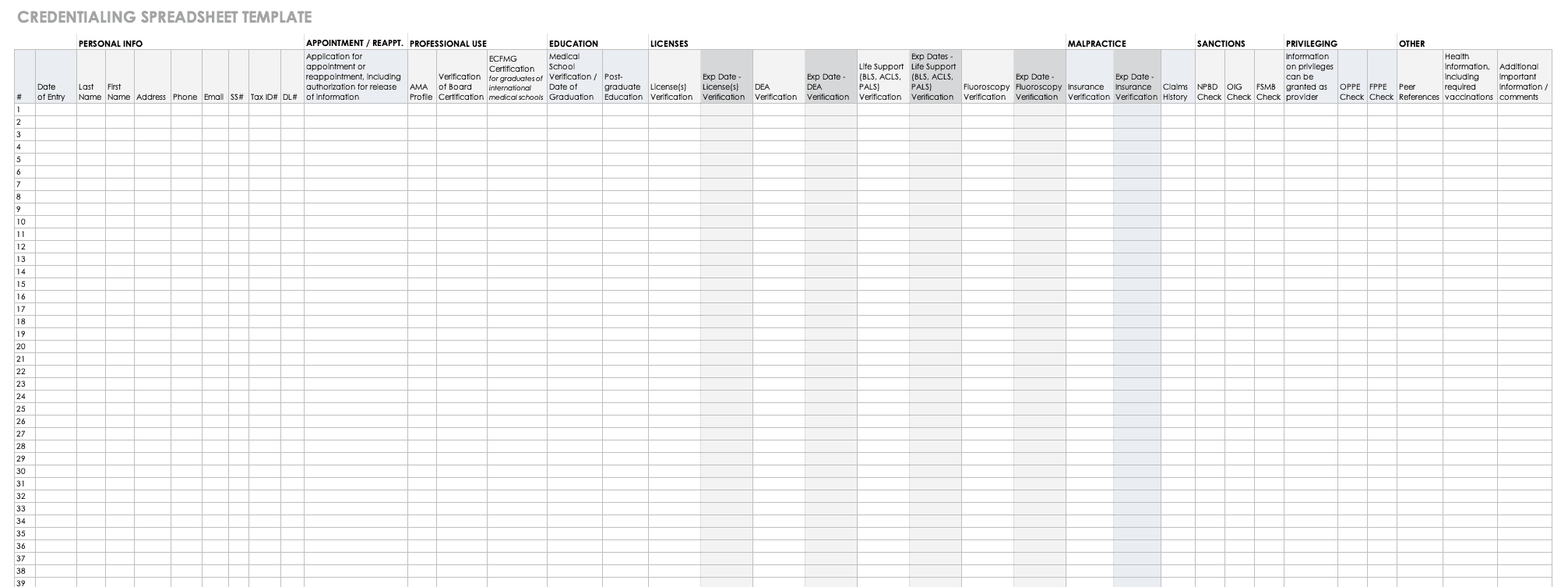
Download Credentialing Spreadsheet Template
What Credentialing Software Can Do
The best credentialing software stores information and can perform services that make the credentialing process easier and more efficient. The software can do the following:
- House large volumes of healthcare provider data in a centralized, secure, and searchable form.
- Eliminate most or all paper — as well as any requirements that providers complete paper forms — from the process.
- Quickly validate credentials and assess qualifications.
- Facilitate virtual meetings for healthcare organizations to assess providers’ credentials.
- Continually track deadlines and renewal requirements for various licenses, certificates, and other medical requirements.
- Automate a wide range of credentialing tasks.
- Help a healthcare organization remain in compliance with industry credentialing regulations and requirements.
- Decrease the time it takes to get a provider credentialed and working.
How to Choose the Right Credentialing Software for Your Organization
Credentialing software can be very helpful for many organizations, but not everyone may need it. Any organization considering credentialing software should assess its needs and understand the realities of how the software operates and is implemented. Here are some questions to ask as you investigate credentialing software:
Why are we considering the software — and why now?
Do the advantages for your organization outweigh the challenges or disadvantages? For instance, think about the time it will take for your staff to learn to use the software, and keep in mind the capabilities and capacity of your information technology (IT) department if you house the software on a local server.
What are other anticipated costs?
What is the return on investment (ROI) you could expect?
Will you need the software for one location or entity, or more than one?
What is a realistic time frame to implement the system?
What level of commitment do you have from key stakeholders, including department and organizational leaders?
Who will be the lead sponsor and project manager within your organization? Who will be in charge of implementing the system?
Features to Look for in Credentialing Software
Many pieces of credentialing software cover the basics. But specific attributes can ensure the software will make a healthcare organization’s credentialing process — and other operations — more effective and efficient.
Among the most important features, the software must have continual digital access to medical licensure boards and similar organizations. Thus, it can automatically track licensing, certificates, and other information about a provider.
“What came to the surface was really around the tracking,” Egbert says. “Who can not only automate my credentialing and help house the data, but who can help my incident reporting or my event reporting — and alert them if there was something that was a red flag” about a provider.
Strong credentialing software should also do the following:
- Provide the option to house the system on the cloud, which means your organization’s representatives — along with providers — can securely access the system from any digital device.
- Integrate with provider credentialing information from the Council for Affordable Quality Healthcare (CAQH). CAQH is a not-for-profit alliance of health insurers that gathers and maintains a repository of provider credentialing information.
- Be able to track and monitor credentials for healthcare providers other than physicians, including nurse practitioners, physician assistants, physical therapists, and mental health providers.
- Automatically give updates and warnings on upcoming expirations of certificates or other renewable credentials.
- Track continuing medical education requirements.
- Incorporate an easy process for peer review, wherein the software solicits, incorporates, and stores feedback about the provider from current and former colleagues.
- Be implemented and learned by staff in a relatively short period.
- Have an easy-to-understand interface, with a dashboard, graphics, and drag-and-drop capabilities.
- Include large amounts of space to store and manage any data that an organization wants to retain about a provider.
- Allow for the use of electronic forms and e-signatures.
- Generate customized reports.
- Integrate with word processing software for the easy creation of letters and documents.
- Integrate with email software for easy communication through the system.
- Track operational metrics by institution, a specific facility location, or a provider.
- Enhance workflow, allowing for the generation of work lists and follow-up requirements.
- Meet credentialing requirements from the Joint Commission and the National Committee on Quality Assurance (NCQA).
- Show hospital privileging information.
- Offer great customer support.
Challenges Associated with Credential Management
A secure credentialing system is vital in healthcare — or any industry that issues credentials for access to information or sites. Significant problems can hit if the system is not properly secured, including the following:
- A hostile party can gain control of the credentialing system and issue false credentials.
- When processes are compromised, the organization may be responsible for the significant expense of reissuing a number of credentials.
- The credentialing system can be the weak link in an organization’s data security, allowing hackers to access providers’ private information and other sensitive data regarding the organization and its partners.
The Advantages and Disadvantages of Cloud-Based Credentialing Software
Because of security concerns, your organization should consider whether you want a cloud-based version of credentialing software or one that operates on your local network.
In a way, your choice is limited. Though some credentialing software offers a choice of cloud-based or on-premises versions, the majority is available only through the cloud as software as a service (SaaS).
With a cloud-based version, anyone in your organization can access the system from anywhere, whether from within different departments or from geographically disparate clinic locations. It also means your medical providers — or prospective providers that your organization is working to credential — can access it wherever they are. As a result, the process can move forward more efficiently than if the software operates only on a local computer server.
The SaaS model also allows the software to be continually updated and improved. That includes keeping up with stringent and continually improved security measures.
Digital security is paramount, of course — especially in the healthcare industry. Larger healthcare organizations may have sufficient IT staffing and feel their data and operations are more secure with on-premises software. Other organizations have built their own versions of credentialing software, and yet more use versions of commercially available software built for local servers.
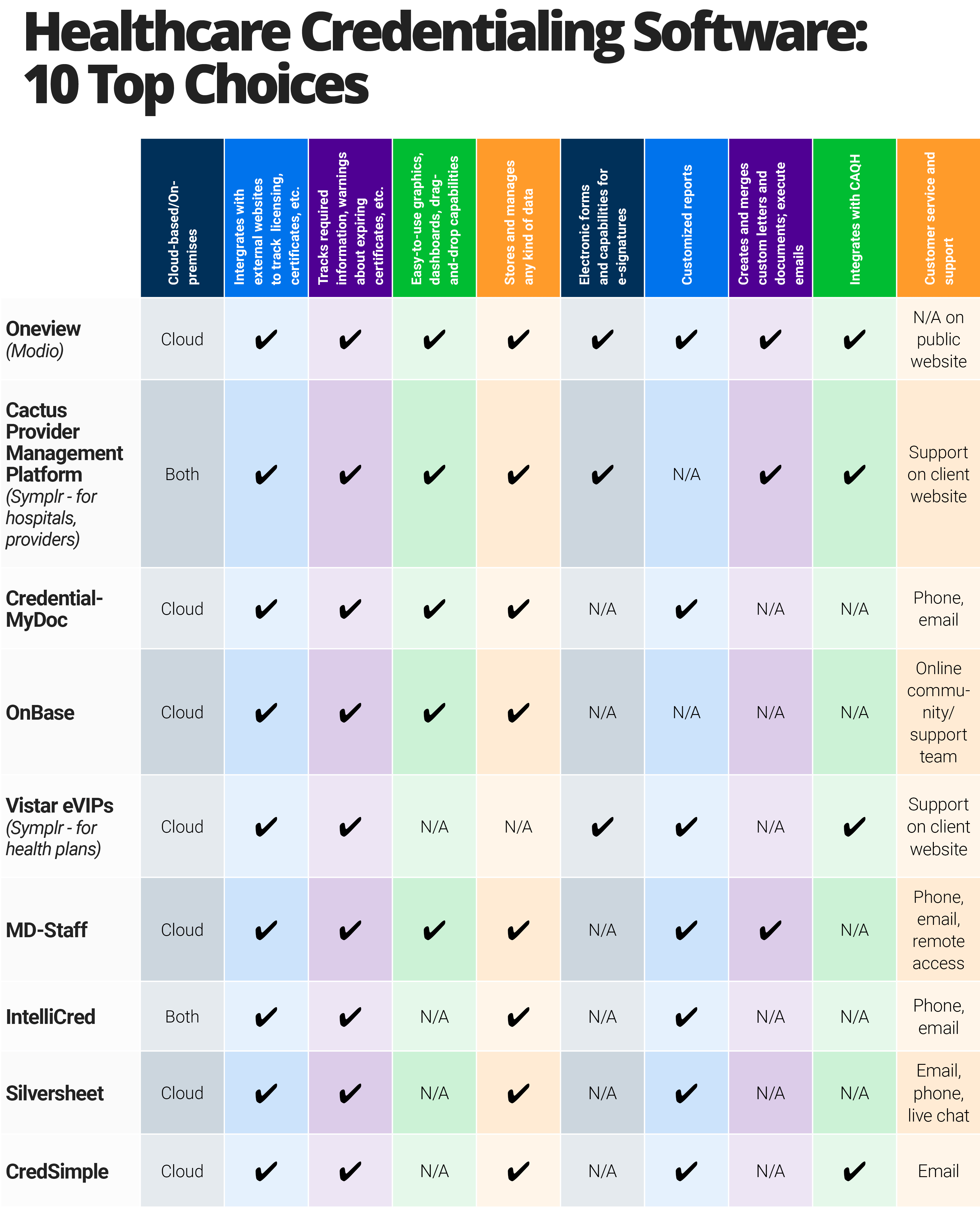
Credentialing Software Matrix
The following chart provides an overview of 10 of the top healthcare credentialing software options available.
Discover a Simple, Efficient Credential Tracking Solution in Smartsheet
Empower your people to go above and beyond with a flexible platform designed to match the needs of your team — and adapt as those needs change.
The Smartsheet platform makes it easy to plan, capture, manage, and report on work from anywhere, helping your team be more effective and get more done. Report on key metrics and get real-time visibility into work as it happens with roll-up reports, dashboards, and automated workflows built to keep your team connected and informed.
When teams have clarity into the work getting done, there’s no telling how much more they can accomplish in the same amount of time. Try Smartsheet for free, today.