What Is Quality Improvement in Healthcare?
In healthcare, quality improvement (QI) refers to the continuous efforts of everyone who is part of the healthcare system to improve care for patients, and to improve the efficiency of the system. The overall goal is to improve people’s health, quicken their recovery from injury or illness, and make sure the system is as efficient and effective as possible.
A range of terms are sometimes used to refer to quality improvement in healthcare, including continuous quality improvement, performance improvement, and quality assurance.
The Benefits of Quality Improvement Processes
The primary benefit of quality improvement in healthcare is — and should be — improved patient health. The goal of everyone who works in the healthcare system is to ensure patients receive the best care possible. This is made possible by working to continually improve how healthcare providers and others in the system do their work.
Mary Jean Schumann is an Associate Professor at the George Washington University School of Nursing and Chair of the Nursing Alliance for Quality Care, a nonprofit group that advocates for quality improvement in healthcare. Ultimately, she says, healthcare quality improvement is about “getting the right care to the right patient at the right time by the right person.”
Another important benefit of quality improvement in healthcare is increased efficiency — and often, cost savings — in the healthcare system.
Other benefits include the following:
- Avoiding significant costs that arise when the system fails, creates an error, or in the worst cases, causes poor outcomes for patients. The first concern is for the patient’s well-being. But, there are other costs, including financial liabilities and damage to a healthcare entity’s reputation.
- Establishing proactive processes that detect and deal with issues before problems occur.
- Helping healthcare organizations transition more easily to new healthcare payment models (set by the federal Centers for Medicare & Medicaid Services [CMS] and insurance companies) that will focus more on patients’ overall health. The new models are replacing the more traditional models of a specific payment for a specific healthcare service. Among new CMS programs is the Merit-based Incentive Payment System (MIPS) and Alternative Payment Model (APM), part of the Quality Payment Program.
- Helping employees of a healthcare organization gain the skills that will then allow the organizations to become part of national quality care programs. Programs include diabetes, heart/stroke, and other programs sponsored by the National Committee for Quality Assurance.
- Helping healthcare organizations earn other recognitions, including the Family Medicine Certification-Performance Improvement activity credit.
- Reducing staff turnover and improving morale — these may be two of the most important benefits.
An Organizational Foundation for Quality Improvement
For the improvement process to be successful, it’s crucial that your organization believes in and establishes some basic principles of quality improvement. The three primary principles that form the foundation of all effective programs are as follows:
- Committed Leadership: Your organization’s CEO or top leader must be committed to the quality improvement process and provide focused leadership toward the goals of the process.
- Understanding Roles: Groups and individual staff members within your organization must understand their role in the process. They must also understand that the hierarchy that may exist within the organization’s clinical care team does not necessarily exist within the quality improvement process or the committee helping to lead it. Roles include a day-to-day project leader, a well-respected healthcare provider “champion” (who works with patients whose care might be affected by the quality improvement program), and people who tabulate and enter data from the program, as well as a separate group that analyzes that data.
- Readiness for Change: Your organization must honestly assess its culture and its willingness to make potentially significant changes to improve care. Do staff members understand the value of quality improvement? Does the organization have structural barriers that will impede the process?
Steps to Implementing a Quality Improvement Program
Your organization can more effectively implement a quality improvement program if it considers some key factors and follows some basic steps:
- Integrate Performance Improvement into Your Strategic Objectives: Make sure that your performance improvement program isn’t at odds with your strategic objectives, and be certain that your strategic objectives provide support for a strong quality improvement program.
- Look for Variations in Your Processes through a Key Process Analysis: The key process analysis focuses on the 80/20 rule — which applies to many industries and economic situations. (It’s also called the Pareto principle.) For the purposes of improving healthcare, it means that 80 percent of the resources needed for a clinical area are driven by 20 percent of the specific care processes. So, focusing on how you perform in one fifth of all care processes can help you quickly become more efficient and effective.
- Ensure You Adjust for Specific Circumstances within the Data: Your providers know why data may vary in specific situations. Take that into account as you consider changes.
- Consider Two Important Factors in Deciding Which Quality Improvement Areas to Tackle First: First, consider the potential return on investment (ROI) in tackling an issue in a specific clinical area. Second, look for the clinical teams that are most open and enthusiastic to the quality improvement process.
- Pick the Permanent Teams: Define the permanent teams that will manage and continue to be part of your quality improvement program.
- Focus on Quality Improvement Areas: Achieve this by using a combination of what the data shows and other factors, like your team members’ experience and openness to the process.
Primary Questions to Answer as You Begin Your Quality Improvement Work
Your organization should begin the quality improvement process by answering some critical questions:
- What Are the Desired Improvements? You should begin by selecting one to three areas of your processes. In selecting these focus areas, think about places where patients or staff have consistent concerns. Or, think about areas of regulatory agency or accrediting agency requirements. You can also consider clinical areas with high volume, where repeated mistakes or issues can cause problems for many patients.
- How Will You Measure Changes and Improvements? Your organization needs to understand which specific data points give a good picture of how a process is working. It then needs to measure that data at the beginning of the improvement process and monitor the same data throughout the process. You will see which — if any — changes occur as the process moves forward, and you may need to make adjustments in reaction to how the data is changing (or, in some cases, not changing).
- How Is Staff Organized to Accomplish the Work? Choose a team of staff members that reflects the various types of jobs involved in a clinical process. The team can be as small as six members (sometimes even fewer). The team can get unwieldy if it gets too large, making it difficult for the team to meet and communicate. All team members, including new members recruited to the team, should show enthusiasm for the process.
- How Can You Leverage Quality Improvement Models to Accomplish Improvements Effectively and Efficiently? You may find that an established model of performing continuous quality improvement can be very helpful. (See more about these models in the following section.)
- How Do You Manage Change? You’ll need to decide whether the changes in the data actually reflect the improvement you’re seeking. Some changes may not reflect real improvements in the process — or improvements that will lead to better patient care. You’ll also want to ensure that beneficial changes in one part of your system are not adversely affecting another part of the system.
One Model for Quality Improvement: The Plan Do Study Act (PDSA) Process
Healthcare organizations use a number of established models to do quality improvement work, including Six Sigma, Lean, and the Plan Do Study Act (PDSA) model. (To learn more about CQI models, check out “CQI in Healthcare: Principles, Process, and Tools.”) Here are some recommended actions from the PDSA model’s four primary components:
- Plan: Establish goals for improvement, identify possible strategies to address the problem, choose specific interventions to implement, and prepare a written plan of action.
- Do: Choose appropriate measures to track, produce visual displays and charts, and assess small components of actions and refine if needed.
- Study: In this phase as well, you will assess small components of actions and refine if needed.
- Act: Identify barriers and determine fixes, identify and use factors that might help facilitate the work (including financial incentives), encourage respected leaders of your team to interact informally with others to stimulate participation in the changes, and communicate internally about the work and its successes.
Tips for Effective Quality Improvement
Experts offer a number of recommendations to make sure your quality improvement process has the best chance for success. Top tips include the following:
- Focus on Improving the System, Not on Individual Mistakes: “Culture is a huge determinant in terms of whether these [efforts] will be effective or not,” says Relias’ Wilson. “If an organization espouses a punitive culture in which people who speak up about mistakes — made by themselves or others — are punished, then systems won’t change.”.
Additionally, she notes, “Caregivers will think if they say anything, they’re going to get blamed.” Therefore, organizational leaders need to establish a culture in which people continually look at improving the systems, rather than punishing people.
- Focus on Outcomes, Not Just Processes: Improving processes can be an important part of quality improvement in healthcare. But, healthcare organizations must be careful not to focus so much on processes that they forget that the final outcomes are ultimately what is most significant.
“It’s always better to measure the outcome, rather than the process,” Lee says. Blood pressure levels, for instance, “are not outcome measures themselves. Outcome measures are factors, such as ‘How does that affect your health?’”
Lee says ultimate outcome measures often relate to overall healthcare quality and financial metrics, or both. - Still Pay Attention to the Underlying Systems: “Still, it’s important to understand the underlying systems that might be causing outcome problems,” says Schumann of the Nursing Alliance for Quality Care.
“The whole point of continuous quality improvement is … you’re looking at the system and why [a problem] is happening,” Schumann explains. “Not just the outcomes — you’re also looking at what the structure and processes are that are making that happen.” - Listen to Patients: “While such advice may seem obvious, healthcare providers often don’t listen carefully to patients and their concerns,” says Schumann, who was a nurse for more than four decades.
“The single most important thing I have found in 50 years in healthcare…is to actually listen to the patient. That will save more medical errors than anything else,” she says. - Clearly Define Your Goals and Your Aims Early — and Stick to Them: “You have to define what it is you’re trying to achieve and what that gap (in measurable indicators) is between the current state and the ideal state,” says Lee.
- Collect Good Baseline Data: You need to know where you are currently in order to set realistic goals for the future.
- Don’t Jump to a Supposed Solution before You’ve Fully Implemented the Quality Improvement Process:
But, she explains, “It’s a big mistake to try to solve the problem before fully understanding the root cause of the problem. When we don’t devote enough time to understanding the root cause and creating a plan — and instead just jump to solutions — I think that’s where teams can run into failures or challenges that are demoralizing.” - Get Buy-In from Your Organization’s CEO and Top Leaders:
- Make Sure Clinical Leaders and Everyday Clinical Staff Are Integrally Involved: Getting clinical staff, especially people who are considered clinical leaders, significantly involved in the process is vital.
“The people who do the work are the ones who inherently have the solutions to the problems,” says Larivee.
“If you don’t have buy-in from your physician groups for a project in a hospital setting, you’re pretty much sunk from the start,” adds Relias Clayton. - Have Someone Responsible for Moving the Project Forward: “Somebody’s got to drive it. Somebody’s got to be accountable for it,” says Relias’ Wilson.
- Track Performance Over Time through Data, and Commit to Ongoing Evaluation and Tracking: “If an organization finds that it has relapses, it’s critical to understand why,” says Larivee. “It’s critical to understand what didn’t work — what went wrong and why. This is where PDSA comes into play. Now that you’ve actually implemented a solution, you’ve got to study it for some period of time,” she notes.
Download Tips for Effective Quality Improvement Checklist
Below are some additional tips from experts:
- Ensure your organization is ready for change and has prepared itself for the process.
- Focus on areas of real importance to your organization, and work to address those areas with clearly designed interventions.
- Ensure your organization provides the necessary financial resources.
- Follow the evidence of what works in healthcare, and make sure your evidence is always up to date.
- Share your successes and lessons learned with everyone in your organization to support broader and more rapid improvements.
- Design your processes to make it easy to do the right thing.
- Consider one-on-one training, where appropriate.
- Focus first on a small number of changes that have a high chance for success.
- Establish a culture of quality in your organization’s systems and structure that support continuous quality improvement.
- Encourage staff reporting of near misses, errors, and hazardous conditions.
- Research what other organizations are doing and collaborate where you can.
- Stay with it. Don’t give up too early.
- Focus on improvement always being part of normal operations. Emphasize the act of continuously trying to improve.
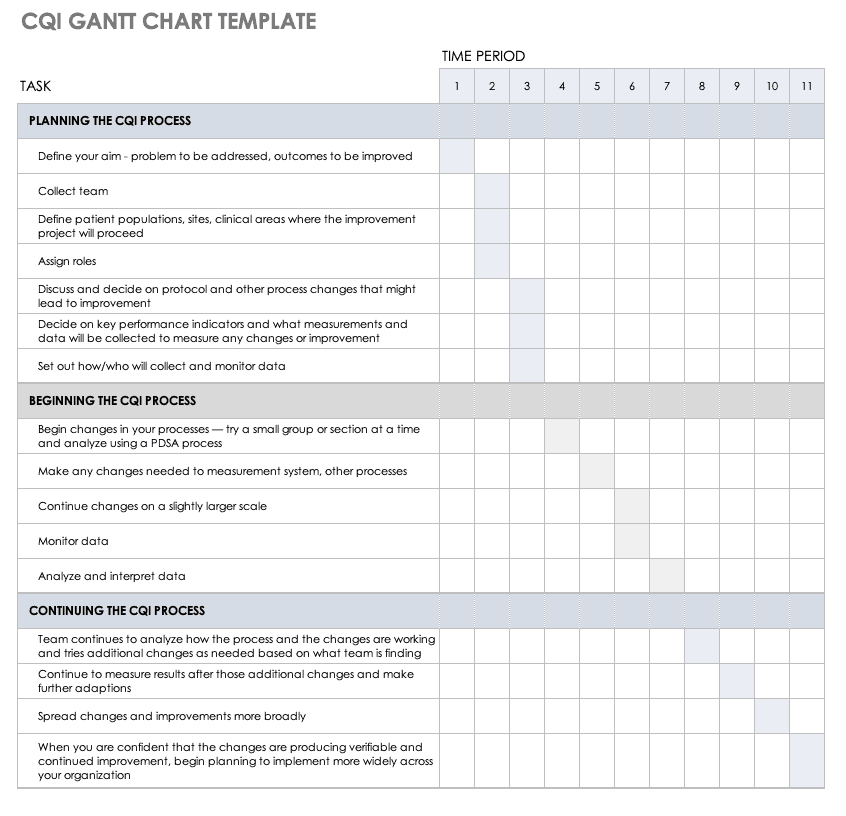
You can also use a Gantt chart as a timeline to track tasks over the course of a project. Use this Gantt chart template, designed specifically for designing and implementing continuous quality improvement initiatives, to monitor your efforts from planning the new process all the way through continuous analysis. This template is free for download and can be customized to fit your needs.
Download Healthcare Quality Improvement Gantt Chart Template
Excel | PDF | Smartsheet
How to Measure Quality Improvement in Healthcare
Possibly the most important aspect of quality improvement is understanding how to measure and track the metrics that reflect how your processes operate. Here are the steps to take:
- Begin planning and understanding how your organization will collect appropriate data.
- Implement a healthcare enterprise data warehouse system that tracks a wide range of data on your processes and procedures.
- Analyze the data to determine the best areas for quality improvement and better efficiencies.
- Produce an honest flow chart that shows your current process. “Note that this is not a flow chart for the ideal process or one that you think should be in place,” Raymond G. Carey, Ph.D. and Rober C. Lloyd, Ph.D. point out in their book Measuring Quality Improvement in Healthcare. As they explain, “Your ability to improve a process will depend on how well you understand the current process and how well your flow chart represents reality.”
- Develop an aim statement (a concise summary of what you hope to achieve over a set duration, including the amount of change you will achieve) to focus your interventions on measurable goals.
- Identify the root cause of a quality issue by using data and quality improvement models.
- Measure progress.
- Have patience: Seeing measurable results can take time.
- Use patient surveys to help assess whether quality is actually improving.
- Develop improvement strategies.
What Is the Purpose of Quality Improvement in Healthcare?
The primary purpose of quality improvement in healthcare is to improve the treatment patients get by identifying the problems in the healthcare system that cause mistakes, fixing those problems, and minimizing those mistakes. A second purpose is to make the system as efficient as possible, which ideally will lower healthcare costs.
Why Is Quality Improvement Important in Healthcare?
Quality improvement is important in any industry or process. However, it’s especially important in healthcare, because people’s lives are continually at stake in a wide range of healthcare procedures and processes. This makes it particularly crucial to improve procedures and minimize the chance of errors.
What Is the Patient Safety and Quality Improvement Act?
Approved in 2005, the Patient Safety and Quality Improvement Act set up a voluntary reporting system that’s meant to provide more information about a range of healthcare quality and patient safety issues. It encourages people to voluntarily report medical errors and other healthcare quality issues. It also offers confidentiality protection to those who provide information.
The Impetus behind Quality Improvement in Healthcare
Medical leaders have been studying and working on what is now called “quality improvement” since at least the 1980s. One of the first pioneers in quality improvement in healthcare was Don Berwick, a pediatrician who was Co-Founder and Co-Principal Investigator of the National Demonstration Project on Quality Improvement in Health Care from 1987 to 1991. In 1991, Berwick co-founded the Institute for Healthcare Improvement.
Quality improvement in healthcare gained a great deal of momentum after the Institute of Medicine published a report entitled “To Err is Human” in 1999. Among other things, the report revealed these statistics:
- Between 44,000 and 98,000 Americans die each year as a result of medical errors.
- Medication errors alone are estimated to cause more than 7,000 deaths annually.
- The total cost of medical errors resulting in injury is estimated to be between $17 billion and $29 billion.
The Institute of Medicine’s Follow-Up Report: “Crossing the Quality Chasm”
Two years after publishing “To Err Is Human,” the Institute of Medicine released a follow-up report entitled “Crossing the Quality Chasm.” It enumerated several overall aims for healthcare quality improvement:
- Safe: Strive to avoid injuries to patients from care that is meant to help them.
- Effective: Provide healthcare services based on scientific knowledge.
- Patient-Centered: Provide care that is responsive to patient preferences.
- Timely: Reduce wait times and potentially harmful delays in treatment.
- Efficient: Avoid waste.
- Equitable: Provide care that isn’t different solely because of the personal characteristics of patients.
The National Strategy for Quality Improvement in Healthcare and Its Aims and Priorities
Later, the federal Affordable Care Act required that the U.S. Department of Health and Human Services (HHS) establish a National Strategy for Quality Improvement in Healthcare. That national strategy was released in March 2011. Its aims and priorities included the following:
- Improving healthcare quality by making it more patient-centered and increasing its reliability, accessibility, and safety
- Improving the overall health of all people through health interventions backed by evidence
- Reducing the cost of good healthcare for people, employers, and government agencies
- Reducing the harms people suffer as a result of the actual delivery of healthcare
- Promoting better communication among providers, and with patients, and better coordination of care
- Encouraging providers to use the best prevention and treatment practices for the illnesses and injuries that cause the most deaths
- Promoting wide use of practices that are healthiest for everyday living
- Making good healthcare more affordable and exploring new ways to deliver care
Overall Goals for Quality Improvement Processes
To reach the overall goals for improved healthcare, healthcare leaders strive for some basic goals regarding how they conduct their healthcare quality improvement processes. Those goals include the following:
- Keep the focus is on patient benefit.
- Leaders and providers should understand that healthcare is delivered as processes within specific systems and, therefore, recognize that they must know how those microsystems work.
- Leaders and providers should know how to measure the effects of an intervention and understand the normal variability in those effects.
- Leaders and providers should collaborate in their quality improvement work.
- Leaders and providers should understand the social context as the quality improvement work advances.
- Leaders and providers should understand that quality improvement is never finished — that it is, quite literally, “continuous” quality improvement.
Other Elements Help Guide and the Improvement Process
Change does not always necessarily mean improvement. In “What Is Quality Improvement and How Can It Transform Healthcare?” a 2007 article in the journal Quality and Safety in Healthcare, Paul Batalden and Frank Davidoff explain that those working on quality improvement need to fully understand the essential aspects of the healthcare process they’re working on. They also need to know the data they’re tracking in order to measure possible improvement. In addition, they need to understand the following:
- The Scientific Evidence: This includes how to use that evidence within the particulars of your processes.
- Context Awareness: This refers to how your providers’ particular habits and traditions play into and affect your processes.
- Performance Measurements: You must know how to use appropriate measures — including time measurements — to understand changes in your process.
- Plans for Change: You must know how to use a range of methods to connect the scientific evidence to the particular process your healthcare entity is trying to improve.
- Execution of Planned Changes: You must know how to use leaders, experts, and resources to bring about positive change.
Pay-for-Performance Programs for Physicians Sometimes Help Improve Healthcare
Some health maintenance organizations and other healthcare organizations have tried pay-for-performance programs to encourage healthcare providers and hospitals to follow evidence-based care standards or other quality improvement strategies.
There are challenges to these arrangements. For example, physicians might seek to avoid especially sick or complicated patients in order to improve their pay-for-performance scores.
However, the arrangements have also shown promise. One study project involving more than 250 hospitals showed that using a pay-for-performance program improved clinical outcomes in five clinical areas: heart failure, acute myocardial infarction (heart attack), coronary artery bypass graft, knee and hip replacement, and pneumonia.
Overall Quality in Healthcare Can Be Evaluated Using Donabedian's Trilogy
Avedis Donabedian, who was born in Beirut, Lebanon and became a researcher and professor at New York Medical College and the University of Michigan, summarized how healthcare quality occurs through what came to be called “Donabedian’s trilogy.” The trilogy refers to three basic components that determine healthcare quality:
- Structure: How the care is organized through the structures of any entity providing healthcare
- Process: How providers work within that structure to try to provide care
- Outcomes: The results that you achieve in patient health (these results are based on the first two components)
Challenges in Quality Improvement in Healthcare
There are many challenges to quality improvement in healthcare, of course. Here are three that most frequently crop up:
- Overall Resistance to Change: This can be particularly present in healthcare because providers feel like they know what has worked before and they worry about risking a patient’s health by making changes.
- Backsliding: A healthcare organization may notice improvement in a healthcare process when the organization as a whole gives significant attention to that process through quality improvement. But, that improvement may wane or reverse as soon as the organization places more focus on a new area of concern.
“You’ll see, as they track [a specific process improvement] month by month, that it goes down as soon as they look in a different direction,” says the Nursing Alliance for Quality Care’s Schumann.
That’s why it’s important, Schumann and others say, to think of quality improvement as an ongoing process, rather than a discretely defined, time-limited project. - Quality Improvement Not Ingrained in the Culture: Quality improvement only works when it becomes an ingrained part of your organization’s structure and culture. It needs to be something everyone in the organization is always thinking about. QI cannot exist as a short-lived project championed by only a few people or a single department.
“The biggest challenge is how to create a culture of CQI,” says Relias’ Clayton. Healthcare is “an overworked, understaffed, stressful environment.” and clinical work alone keeps people perpetually busy. Sometimes, then, quality improvement “becomes a department… it’s a person or two or three people that are over there doing a project, trying to collect information to meet some board requirement. So, it’s not actually inculcated in the culture and the heart and soul of the organization,” explains Clayton.
Additional challenges in QI in healthcare include the following:
- When an organization is unable to select improvement goals that fit within its strategic priorities, the effort doesn’t have the support to succeed.
- There is not enough ongoing training and skills development to support the process.
- There are not direct and clear expectations.
- Leaders of an organization are not involved or engaged.
- There is not enough devotion to assessing and tracking credible data.
Challenges in Measuring Continuous Quality Improvement Results
Beyond overall challenges in quality improvement programs, there are also challenges in evaluating and measuring change and possible improvement. These challenges include the following:
- Medical providers often don’t completely understand the causes and effects for many health conditions. Treatment often relies on physician experience and judgments — and those factors are difficult to measure.
- There is limited scientific evidence that links certain processes to specific patient outcomes.
- It is sometimes difficult to rule out alternative explanations for results because patients present so many correlated and interrelated variables.
- Measures on patient outcomes are heavily influenced by the mix of patients a healthcare organization treats, including their income levels, health histories, past access to healthcare, etc.
- Sample sizes are too small to properly assess whether the changes have helped.
- Data from clinical care is often incomplete or inaccurate.
- Healthcare organizations experience technological and other general problems in how they measure organizational performance.
- Self-measurements of results can be different from measurements made by a disinterested outside entity.
Healthcare and small business consultant Lee says he’s watched organizations that, “according to their own measures, look great.” But, when they use a third party to validate the results, he says they realize that they “[Are] not as great as [they] thought [they] were.”
Government Agencies and Other Organizations Have Established Healthcare Quality Improvement Measures and Guidance
A range of governmental agencies and other organizations have established measures or standards that guide quality improvement work or quality healthcare in general. They include the following:
National data sets also help assess healthcare quality and guide quality improvement. Here are two valuable sets:
The National Healthcare Quality and Disparities Report
To assess how healthcare providers were dealing with some of the issues outlined by the Department of Health and Human Services’ National Strategy for Quality Improvement in Health Care, a report called the National Healthcare Quality and Disparities Report (NHQDR) was published in 2014. It found that progress had been made in each of the priorities outlined by HHS. But, it also found continuing issues.
Among other things, the report found the following:
- Only 70 percent of people with high blood pressure were receiving the recommended level of care.
- Disparities increased in hospice care and chronic disease management.
- Healthcare affordability was still an issue. Costs were leveling off, but were not yet decreasing.
Future Trends in Healthcare Quality Improvement
Experts are starting to see trends in how quality improvement work is being performed that may accelerate in the future. Those trends include the following:
- Medical training using augmented reality
- A significantly increased use of data in healthcare
- An increase in personalized medicine, along with the personalization of a patient’s clinical care experience, based on their preferences
- An increased use of wearable devices to monitor health
- An increased use of smart technology in hospitals
- An increased use of artificial intelligence (AI) and the internet of things (IoT) in healthcare
- An increased interest in the health management of the general population or large groups of people (for instance, everyone with heart disease)
- Advanced technology that will increase overall healthcare efficiency
Tools to Help With Quality Improvement
There are a number of useful tools available for working on quality improvement:
- Diagrams that illustrate process flow, the interrelationship among processes, and cause and effect.
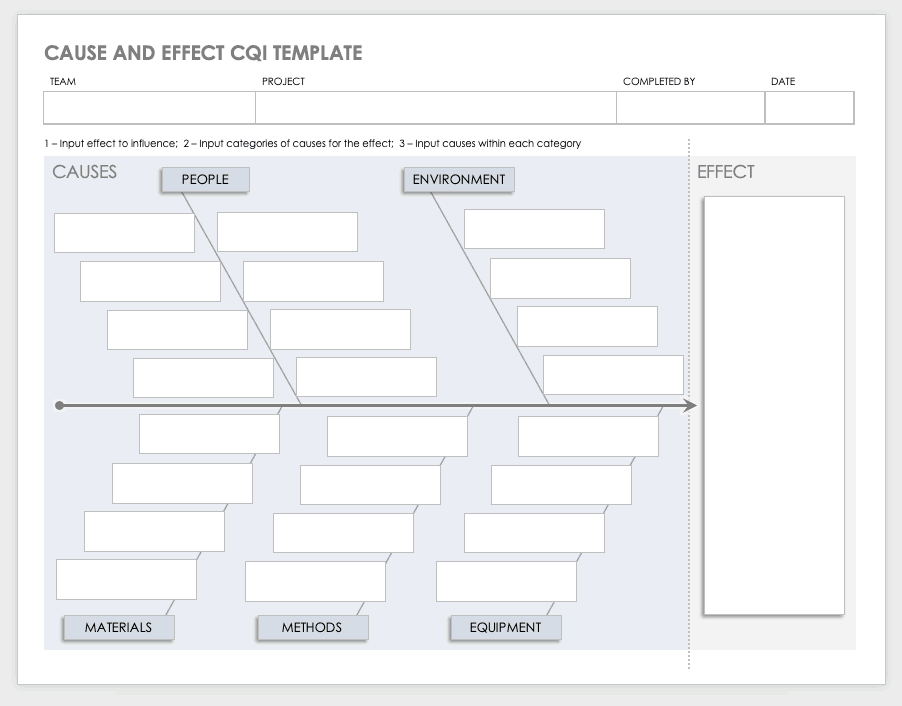
Use this cause and effect template to diagram people, environment, materials, methods, and equipment, and the effects that these factors have on the rest of the project, and your long term goals. This template is free to download and fully customizable.
Download Cause and Effect Diagram
- Diagrams that show how positive change might be driven through actions
- A failure modes and effects analysis (FMEA), used in Six Sigma
- A histogram, which is a bar chart that helps teams analyze variations in a measurement
- A Pareto chart, which is used to illustrate the Pareto principle
- A PDSA worksheet
- A project planning form
- A run chart, which is a graph of data over time
- A scatter diagram or scatter plot, which is a graph with an X and Y axis that represents the relationship between two variables
Quality Improvement in Healthcare with Smartsheet for Healthcare
Empower your people to go above and beyond with a flexible platform designed to match the needs of your team — and adapt as those needs change.
The Smartsheet platform makes it easy to plan, capture, manage, and report on work from anywhere, helping your team be more effective and get more done. Report on key metrics and get real-time visibility into work as it happens with roll-up reports, dashboards, and automated workflows built to keep your team connected and informed.
When teams have clarity into the work getting done, there’s no telling how much more they can accomplish in the same amount of time. Try Smartsheet for free, today.